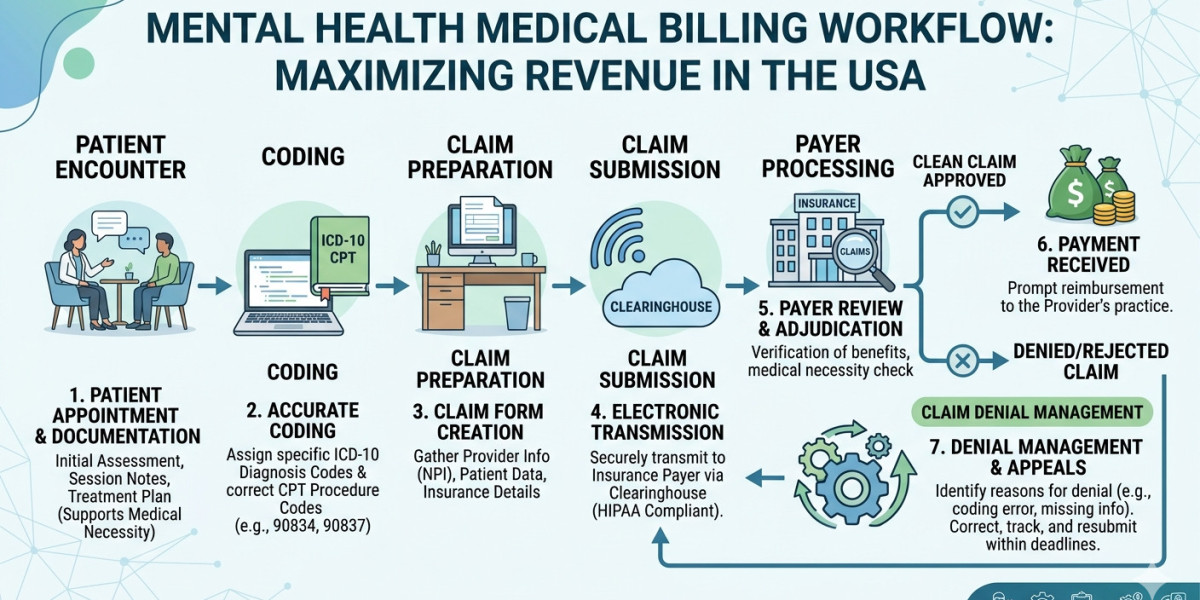
Mental health practices across the USA are experiencing unprecedented demand. Therapists, psychiatrists, psychologists, and behavioral health clinics are helping more patients than ever before, yet many providers still struggle with one major operational challenge—billing.
From claim denials and coding errors to insurance verification delays and compliance issues, the administrative side of behavioral healthcare can quickly become overwhelming. That’s why efficient mental health medical billing has become a critical part of maintaining financial stability while continuing to deliver quality patient care.
Whether you run a private therapy practice or manage a multi-provider behavioral health clinic, understanding how modern billing systems work can significantly improve reimbursements, reduce administrative stress, and strengthen your overall revenue cycle.
Why Mental Health Billing Is More Complex Than Other Medical Specialties
Behavioral health billing is unique. Unlike many traditional medical specialties, mental health providers often deal with:
- Time-based CPT codes
- Frequent authorization requirements
- Telehealth compliance updates
- Changing payer policies
- Session limitations
- Complex documentation standards
Even a small mistake in coding or claim submission can delay payments for weeks.
For example, a therapist may correctly document a 60-minute psychotherapy session but accidentally submit the wrong CPT code modifier. The payer rejects the claim, forcing staff to resubmit and follow up repeatedly. Over time, these issues create cash flow disruptions and administrative burnout.
This is why many practices now work with a dedicated mental health billing specialist or partner with experienced behavioral health billing teams.
The Growing Demand for Mental Health Insurance Billing Services
Insurance companies have become increasingly strict about behavioral health reimbursements. Payers now require:
- Accurate diagnosis coding
- Proper session documentation
- Timely filing compliance
- Prior authorization verification
- Correct telehealth modifiers
As regulations evolve, providers are turning to professional mental health insurance billing services to reduce errors and improve collections.
A strong billing process does more than submit claims. It ensures every stage of reimbursement is optimized, including:
Front-End Verification
Before appointments occur, insurance eligibility and benefits must be confirmed accurately.
Coding Accuracy
Behavioral health coding requires deep familiarity with psychotherapy CPT codes, ICD-10 diagnoses, and payer-specific rules.
Claims Management
Clean claims improve first-pass acceptance rates and minimize delays.
Denial Resolution
Appealing denied claims requires persistence, payer knowledge, and documentation expertise.
Payment Posting and Reporting
Financial transparency helps providers monitor profitability and identify revenue leaks.
Common Billing Challenges Mental Health Providers Face
Many behavioral health practices unknowingly lose revenue because of avoidable billing mistakes.
Here are some of the most common issues:
Incorrect Time-Based Coding
Mental health services are often billed based on session duration. If documentation doesn’t support the billed time, claims may be rejected.
Authorization Failures
Some insurance plans require pre-authorization for therapy sessions or psychiatric services. Missing approvals can result in denied reimbursements.
Telehealth Billing Errors
Virtual therapy has transformed behavioral healthcare, but payer guidelines continue to change. Incorrect telehealth modifiers can create payment delays.
Incomplete Documentation
Insurance companies frequently audit behavioral health claims. Missing treatment notes or insufficient documentation can trigger denials.
Credentialing Delays
Without proper enrollment and payer credentialing, providers may experience lengthy reimbursement interruptions.
This is why many clinics seek support from a reliable mental health billing consultant who understands payer policies and compliance requirements.
Why Practices Choose to Outsource Mental Health Billing Services
Administrative workloads can quickly overwhelm in-house staff. Managing scheduling, patient communication, insurance verification, coding, and collections simultaneously often leads to inefficiencies.
As a result, more practices now outsource mental health billing services to experienced behavioral health billing professionals.
Benefits of Outsourced Mental Health Billing
Improved Claim Accuracy
Experienced billing teams understand behavioral health coding nuances and payer-specific requirements.
Faster Reimbursements
Clean claims reduce delays and improve cash flow consistency.
Reduced Administrative Burden
Therapists and office staff can focus more on patient care instead of chasing unpaid claims.
Better Denial Management
Professional billing teams identify denial trends and resolve issues proactively.
Scalability
Growing practices can handle larger patient volumes without hiring additional in-house billing staff.
A dependable mental health billing services agency can help practices streamline operations while improving financial performance.
What Makes the Best Mental Health Billing Agency Stand Out?
Not all billing companies specialize in behavioral health. Choosing the right partner requires careful evaluation.
The best mental health billing agency typically offers:
- Behavioral health-specific expertise
- HIPAA-compliant workflows
- Dedicated account management
- Insurance verification support
- Denial management services
- Telehealth billing expertise
- Customized reporting dashboards
An experienced mental health billing provider should also stay updated on changing payer policies and compliance regulations.
The Role of Coding in Mental Health Reimbursement
Coding directly impacts reimbursement success. Accurate coding ensures providers are properly compensated for the services delivered.
Behavioral health coding often includes:
- Psychotherapy sessions
- Family therapy
- Group therapy
- Psychiatric evaluations
- Medication management
- Crisis intervention services
A qualified mental health billing and coding company understands how to align documentation with payer expectations.
Errors in coding can lead to:
- Claim denials
- Underpayments
- Compliance audits
- Revenue leakage
That’s why practices increasingly rely on professional mental health medical billing services with specialized coding expertise.
Real-World Example: How Outsourced Billing Improved Revenue
A mid-sized behavioral health clinic in Texas struggled with frequent denials related to telehealth claims. Their internal administrative staff lacked the time to monitor changing payer rules.
After transitioning to an outsourced mental health billing team, the clinic implemented:
- Real-time eligibility verification
- Correct telehealth modifiers
- Automated claims tracking
- Faster denial appeals
Within six months, the clinic reported:
- Higher first-pass claim acceptance rates
- Reduced accounts receivable days
- Improved monthly collections
- Lower administrative stress
This example highlights why many practices now seek a top outsource mental health billing company to strengthen revenue cycle performance.
How Technology Is Changing Mental Health Medical Billing
Modern billing systems are transforming behavioral healthcare operations.
Today’s advanced mental health medical billing solution platforms often include:
Automated Claims Scrubbing
Claims are checked for errors before submission.
Real-Time Eligibility Checks
Insurance coverage can be verified instantly.
Integrated EHR Systems
Documentation and billing workflows become more efficient.
Analytics and Reporting
Providers gain visibility into collections, denials, and payer performance.
Telehealth Billing Support
Updated coding tools improve virtual care reimbursement accuracy.
Technology alone isn’t enough, however. Successful outcomes still depend on knowledgeable billing experts who understand behavioral healthcare regulations.
Why Mental Health Therapists Need Specialized Billing Support
Independent therapists often face unique billing challenges. Many clinicians enter private practice without extensive insurance billing experience.
Professional billing services for mental health therapists help simplify complicated administrative tasks such as:
- Insurance claim submission
- Benefit verification
- Copayment tracking
- Denial follow-up
- Credentialing support
This allows therapists to spend more time helping patients instead of managing paperwork.
Similarly, larger organizations benefit from customized billing services for mental health providers that align with practice size, specialty focus, and payer mix.
Credentialing Matters More Than Most Practices Realize
Credentialing delays can seriously impact cash flow.
Before providers can bill insurance companies, they must complete enrollment and credentialing processes with each payer network. Errors or missing documentation often create lengthy delays.
Many practices now combine credentialing services with their billing workflows to ensure smoother onboarding and faster reimbursements.
Efficient credentialing also supports:
- Faster payer approvals
- Reduced claim rejections
- Expanded insurance participation
- Better patient accessibility
Revenue Cycle Management Is Essential for Long-Term Growth
Successful mental health practices do more than submit claims. They build strong financial systems that support sustainable growth.
Comprehensive revenue cycle management services help optimize every stage of the reimbursement process, including:
- Patient scheduling
- Eligibility verification
- Charge capture
- Coding accuracy
- Claims submission
- Payment posting
- Denial management
- Patient collections
Strong revenue cycle management reduces revenue leakage while improving operational efficiency.
Choosing the Right Mental Health Billing Company
Before selecting a billing partner, providers should evaluate several factors carefully.
Questions to Ask:
- Does the company specialize in behavioral health?
- How do they manage denied claims?
- What reporting tools are available?
- Do they support telehealth billing?
- Can they assist with credentialing?
- What is their average claim acceptance rate?
The right professional mental health billing company should function as a long-term operational partner rather than simply a claim submission vendor.
Why Specialized Medical Billing Expertise Matters
Mental health providers increasingly need billing partners who understand both financial operations and healthcare compliance.
Companies offering:
- medical billing services
- medical coding services
- medical billing and coding services
- revenue cycle management services
- credentialing services
can provide integrated support that improves efficiency across the entire practice.
When billing, coding, and compliance work together seamlessly, providers can reduce administrative pressure while strengthening profitability.
How 247 Medical Billing Services Supports Behavioral Health Providers
Many behavioral health practices across the USA are now seeking specialized operational support to navigate growing reimbursement complexities.
Experienced organizations like 247 Medical Billing Services provide tailored solutions for behavioral health providers through:
- Mental health insurance billing support
- Behavioral health coding expertise
- Revenue cycle optimization
- Credentialing assistance
- Denial management strategies
- End-to-end medical billing and coding services
With the right systems and experienced professionals in place, mental health providers can focus more on patient care while maintaining healthier financial performance.
Conclusion
The future of behavioral healthcare depends not only on quality patient care but also on operational efficiency. As insurance requirements become more complex, effective mental health medical billing has become essential for maintaining profitability and reducing administrative strain.
Whether providers choose in-house support or decide to outsource mental health billing services, the goal remains the same: cleaner claims, faster reimbursements, and fewer denials.
By combining accurate coding, strong compliance practices, advanced billing technology, and comprehensive revenue cycle strategies, mental health providers across the USA can build sustainable practices that continue serving patients effectively for years to come.
FAQs
What is mental health medical billing?
Mental health medical billing involves submitting and managing insurance claims for behavioral health services such as therapy, psychiatry, counseling, and psychological evaluations.
Why do providers outsource mental health billing services?
Many providers outsource billing to improve claim accuracy, reduce denials, speed up reimbursements, and minimize administrative workload.
What does a mental health billing specialist do?
A mental health billing specialist handles insurance verification, coding, claims submission, denial management, payment posting, and reimbursement follow-up for behavioral health practices.
How can a mental health billing agency improve revenue?
A specialized billing agency helps reduce claim errors, improve clean claim rates, manage denials effectively, and optimize revenue cycle performance.
Are credentialing services important for mental health providers?
Yes. Credentialing ensures providers are enrolled with insurance payers correctly, which helps prevent claim rejections and reimbursement delays.
What should providers look for in a mental health billing company?
Providers should choose a company with behavioral health expertise, HIPAA compliance knowledge, denial management experience, telehealth billing support, and transparent reporting systems.